Forte for Perioperative Nutritional Support in the Perioperative Period
Introduction
The preoperative assessment of both sarcopenia, malnutrition, and high arginase states is increasingly recognized as important adjunct in risk reduction for patients undergoing major gastrointestinal (GI) surgery in enhanced recovery programs (ERP). At least 10 metaanalyses regarding the assessment of immunonutrition have been published, however, virtually all of the data is from a period of time to adoption for ERP’s. This gap is highlighted by the metaanalysis peformed by Hegazi which assessed 8 randomized controlled trials (RCTs) of preoperative immunonutrition (IN) vs. standard enteral therapy were identified and 9 RCTs of IN vs. no supplements. The authors concluded that there is no advantage of IN over standard protein supplementation.
Similarly, comparing two recent studies demonstrates the same conundrum regarding the benefits of supplement components within an ERP:
- Moya et al- randomized patients into receiving no supplement versus IN and reported a reduction in surgical site infection in the absence of a mechanical/antibiotic bowel prep.
- Huber et al randomized elective major GI surgery between IN or isocaloric isonitrogenous nutrition (ICN) given for 5 days preoperatively within an ERAS pathway which demonstrated no improvement in outcomes.
These data are further complicated by recent data suggesting that glutamine and omega 3 fatty acids are either associated with increased risk or no benefit in many stressed patient populations. Therefore, there remains a significant gap in the appropriate supplement components based on modern assessment of nutritionally at risk surgical patients and the impact of a better formulation on functional outcomes.
Modern Assessment of Nutritionally at Risk Surgical Patients
The current evidence-based investigations capable of assessing this at risk surgical patients include:
- CT measured sarcopenia scores
- Ultrasound assessment of rectus femoris size
- Nutritional metabolic scores (Prognostic Nutritional Index and Glasgow Prognostic Score)
- Assessement of systemic arginine bioavailability (systemic methylarginines, ornithine:citrulline ratio, and proline:citrulline ratio).
These data are easily and economically efficient means of assessing preoperative nutritional and immunologic impairment of major surgical patients. Clinicians should strongly consider routine application of some of these strategies within their ERP. The PNI has consistently demonstrated efficacy in highlighting patients with poor short and long term outcomes, especially with oncologic surgery.
Surgical Stress Impact on Arg/ADMA and use of L-Citrulline Versus Enteral Arginine and Glutamine
The surgical stress response also induces a decrease in arginine (Arg) bioavailability and an increase in asymmetric dimethyl arginine which is an natural inhibitor of arginine associated nitric oxide function. The net result is a lowering of the Arg/ADMA ratio in the early postoperative period and is associated with increased SSI rates, cardiovascular complications, and acute kidney injury.
A reduced arg/ADMA ratio has been demonstrated to correlate with poor outcomes in a variety of settings of physiologic stress including cardiac and non-cardiac surgery, acute coronary syndrome, stroke, and sepsis. Echeloef et al recently confirmed the negative impact of perioperative reduction in arginine bioavailability on endothelial dysfunction in colectomy.
Acute and chronic elevations in serum glucose also work to lower this ratio. LCitrulline has recently and consistently been demonstrated to safely and effectively restore systemic arginine levels and reduce ADMA in a variety of clinical scenarios. L-Citrulline is virtually 100% absorbed by the intestine and subsequently, virtually 100% is converted to arginine for systemic utilization. Conversely, surgical stress increases the function of constituitively active hepatic arginase which degrades a significant component of enterally administered arginine, rendering it inactive.
Similarly, the principal potential benefit of enteral glutamine appears to be related to enterocyte conversion to citrulline which is absorbed and converted to arginine. Therefore, it is simply more efficient to provide the superior biologic precursor, L-Citrulline, to enhance the systemic arginine/ADMA ratio as well as the ornithine:citrulline ratio, and proline:citrulline ratios. The higher degree of bioavalibility of systemic arginine is also important because of its ultimate conversion to ornithine and then proline which supports wound healing via collagen formation. Higher doses of arginine are required to support similar systemic levels but
Negative Impact of High Carbohydrate to Protein Ratios in Sarcopenic States
It appears that moderate-to-large servings of protein or amino acids increases muscle protein synthesis similarly in both young and elderly, especially in ranges of 10 and 20g per servings of essential amino acids. However, Volpi et al demonstrated that co-ingestion of protein and relatively large amounts of simple carbohydrate markedly diminishes the benefit of protein supplementation in sarcopenic elderly patients.
As a result of this research, we have significantly reduced the amount of carbohydrates and provided those calories in the form of a complex carbohydrate (maltodextrin). In addition, Forte is enriched with whey protein isolate to supply the more beneficial branch chain amino acid leucine to further enhance the impact of protein supplementation on muscle protein synthesis. Vitamin K2 has also demonstrated an adjunctive role with respect to muscle protein synthesis in sarcopenic patients and this is included at a level associated with improved protein utilization.
Vitamin K2 has demonstrated efficacy in improving cardiac output even with short term supplementation.
Summary
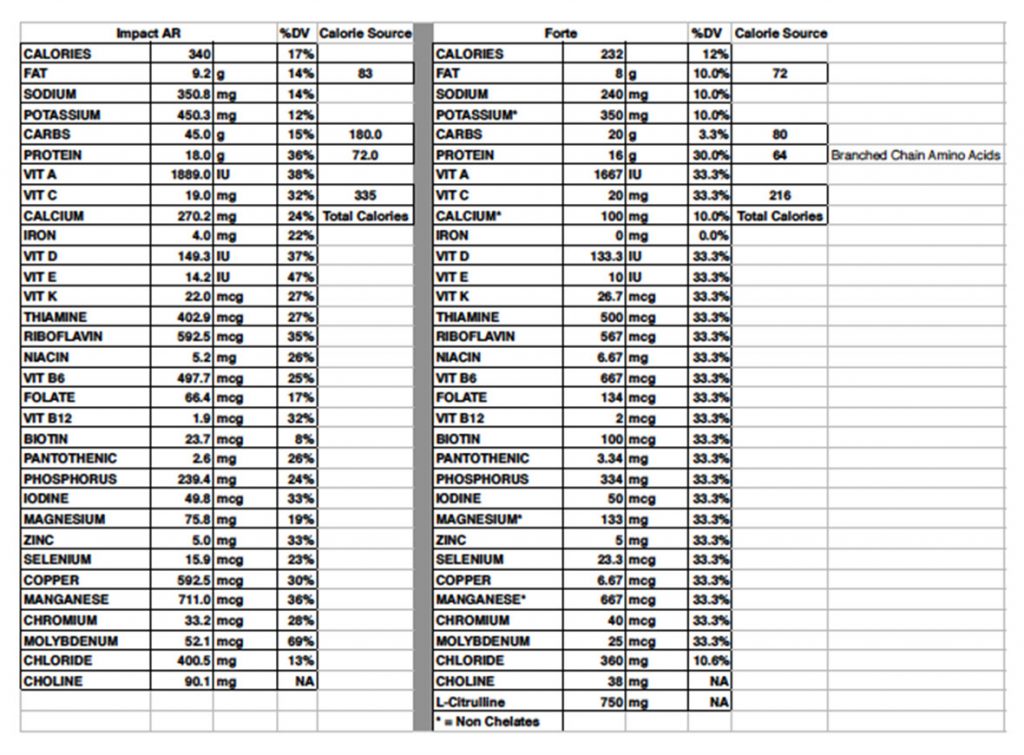
The table below demonstrates the differences between Forte and the typically recommended Impact AR. We believe the reduction in simple carbohydrates and the use of complex carbohydrate is superior. Complex carbohydrates appear efficient in inducing insulin sensitivity. Reliance upon whey protein provides a robust branch chain amino acid, especially leucine. Substitution of Citrulline for arginine and the additional supplementation with vitamin D and K2 offer an excellent, evidence-based option for the preoperative care of the nutritionally-at-risk surgical population.
Selected References
Sarcopenia and Maltnurition
1: Lieffers JR, Bathe OF, Fassbender K, Winget M, Baracos VE. Sarcopenia is
associated with postoperative infection and delayed recovery from colorectal
cancer resection surgery. Br J Cancer. 2012 Sep 4;107(6):931-6.
2: Peng P, Hyder O, Firoozmand A, Kneuertz P, Schulick RD, Huang D, Makary M,
Hirose K, Edil B, Choti MA, Herman J, Cameron JL, Wolfgang CL, Pawlik TM. Impact
of sarcopenia on outcomes following resection of pancreatic adenocarcinoma. J
Gastrointest Surg. 2012 Aug;16(8):1478-86.
3: Sheetz KH, Waits SA, Terjimanian MN, Sullivan J, Campbell DA, Wang SC,
Englesbe MJ. Cost of major surgery in the sarcopenic patient. J Am Coll Surg.
2013 Nov;217(5):813-8.
4: Cederholm T, Jensen GL. To create a consensus on malnutrition diagnostic
criteria: A report from the Global Leadership Initiative on Malnutrition (GLIM)
meeting at the ESPEN Congress 2016. Clin Nutr. 2016 Dec 16. pii:
S0261-5614(16)31342-5.
5: Sánchez-Rodríguez D, Marco E, Ronquillo-Moreno N, Miralles R, Vázquez-Ibar O,
Escalada F, Muniesa JM. Prevalence of malnutrition and sarcopenia in a post-acute
care geriatric unit: Applying the new ESPEN definition and EWGSOP criteria. Clin
Nutr. 2016 Sep 9. pii: S0261-5614(16)30233-3.
6: McFarlin BK, Henning AL, Venable AS. Oral Consumption of Vitamin K2 for
8 Weeks Associated With Increased Maximal Cardiac Output During Exercise.
Altern Ther Health Med. 2017 Jul;23(4):26-32.
Preoperative Carbohydrate Loading
1: Singh BN, Dahiya D, Bagaria D, Saini V, Kaman L, Kaje V, Vagadiya A, Sarin S,
Edwards R, Attri V, Jain K. Effects of preoperative carbohydrates drinks on
immediate postoperative outcome after day care laparoscopic cholecystectomy. Surg
Endosc. 2015 Nov;29(11):3267-72. doi: 10.1007/s00464-015-4071-7. Epub 2015 Jan
22. PubMed PMID: 25609319.
2: Bilku DK, Dennison AR, Hall TC, Metcalfe MS, Garcea G. Role of preoperative
carbohydrate loading: a systematic review. Ann R Coll Surg Engl. 2014
Jan;96(1):15-22. doi: 10.1308/003588414X13824511650614. Review. PubMed PMID:
24417824.
3: Ljunggren S, Hahn RG, Nyström T. Insulin sensitivity and beta-cell function
after carbohydrate oral loading in hip replacement surgery: a double-blind,
randomised controlled clinical trial. Clin Nutr. 2014 Jun;33(3):392-8. doi:
10.1016/j.clnu.2013.08.003. Epub 2013 Aug 15. PubMed PMID: 24007934.
4: Li L, Wang Z, Ying X, Tian J, Sun T, Yi K, Zhang P, Jing Z, Yang K.
Preoperative carbohydrate loading for elective surgery: a systematic review and
meta-analysis. Surg Today. 2012 Jul;42(7):613-24. doi: 10.1007/s00595-012-0188-7.
Epub 2012 May 13. Review. Erratum in: Surg Today. 2012 Nov;42(11):1142. PubMed
PMID: 22581289.
5: Ljungqvist O. Modulating postoperative insulin resistance by preoperative
carbohydrate loading. Best Pract Res Clin Anaesthesiol. 2009 Dec;23(4):401-9.
Review. PubMed PMID: 20108579.
Reduced Maltodextrin Dose
1: Faria MS, de Aguilar-Nascimento JE, Pimenta OS, Alvarenga LC Jr,
Dock-Nascimento DB, Slhessarenko N. Preoperative fasting of 2 hours minimizes
insulin resistance and organic response to trauma after video-cholecystectomy: a
randomized, controlled, clinical trial. World J Surg. 2009 Jun;33(6):1158-64.
doi: 10.1007/s00268-009-0010-x. PubMed PMID: 19363695.
Arg/ADMA ratio Impact
1: Mortensen KM, Itenov TS, Haase N, Müller RB, Ostrowski SR, Johansson PI, Olsen
NV, Perner A, Se-Jensen P, Bestle MH. High Levels of Methylarginines Were
Associated with Increased Mortality in Patients with Severe Sepsis. Shock. 2016
May 19. [Epub ahead of print] PubMed PMID: 27206279.
2: Willeit P, Freitag DF, Laukkanen JA, Chowdhury S, Gobin R, Mayr M, Di
Angelantonio E, Chowdhury R. Asymmetric dimethylarginine and cardiovascular risk:
systematic review and meta-analysis of 22 prospective studies. J Am Heart Assoc.
2015 May 28;4(6):e001833. doi: 10.1161/JAHA.115.001833. Review. PubMed PMID:
26021436; PubMed Central PMCID: PMC4599532.
3: Rowland MR, Ragina NP, Sarkar J, Uyehara CF, Senagore AJ. Is
arginine/asymetric dimethylarginine ratio depletion an indicator of insufficient
resuscitation in a porcine model of hemorrhage-reperfusion? Surgery. 2014
Oct;156(4):861-8. doi: 10.1016/j.surg.2014.06.019. PubMed PMID: 25239335.
4: Molnar T, Pusch G, Papp V, Feher G, Szapary L, Biri B, Nagy L, Keki S, Illes
Z. The L-arginine pathway in acute ischemic stroke and severe carotid stenosis:
temporal profiles and association with biomarkers and outcome. J Stroke
Cerebrovasc Dis. 2014 Sep;23(8):2206-14. doi: 10.1016?j.jstrokecerebrovasdis. 2014.05.002. Epub 2014 Jul 10. PubMed PMID:25018114.
5: Lindgren C, Hultin M, Koskinen LO, Lindvall P, Borota L, Naredi S. ADMA levels
and arginine/ADMA ratios reflect severity of disease and extent of inflammation
after subarachnoid hemorrhage. Neurocrit Care. 2014 Aug;21(1):91-101. doi:
10.1007/s12028-013-9945-8. PubMed PMID: 24408146.
6: Brinkmann SJ, de Boer MC, Buijs N, van Leeuwen PA. Asymmetric dimethylarginine
and critical illness. Curr Opin Clin Nutr Metab Care. 2014 Jan;17(1):90-7. doi:
10.1097/MCO.0000000000000020. Review. PubMed PMID: 24281375.
7: Betz B, Möller-Ehrlich K, Kress T, Kniepert J, Schwedhelm E, Böger RH, Wanner
C, Sauvant C, Schneider R. Increased symmetrical dimethylarginine in ischemic
acute kidney injury as a causative factor of renal L-arginine deficiency. Transl
Res. 2013 Aug;162(2):67-76. doi: 10.1016/j.trsl.2013.04.005. Epub 2013 May 22.
PubMed PMID: 23707198.
8: Maas R, Dentz L, Schwedhelm E, Thoms W, Kuss O, Hiltmeyer N, Haddad M, Klöss
T, Standl T, Böger RH. Elevated plasma concentrations of the endogenous nitric
oxide synthase inhibitor asymmetric dimethylarginine predict adverse events in
patients undergoing noncardiac surgery. Crit Care Med. 2007 Aug;35(8):1876-81.
PubMed PMID: 17581491.
9:Ekeloef S, Larsen MH, Schou-Pedersen AM, Lykkesfeldt J, Rosenberg J, Gögenür I. Endothelial dysfunction in the early postoperative period after major colon cancer surgery. Br J Anaesth. 2017 Feb;118(2):200-206.
Citrulline Impact in Acute Stress/Supplementation
1: Wijnands KA, Meesters DM, van Barneveld KW, Visschers RG, Briedé JJ,
Vandendriessche B, van Eijk HM, Bessems BA, van den Hoven N, von Wintersdorff CJ,
Brouckaert P, Bouvy ND, Lamers WH, Cauwels A, Poeze M. Citrulline Supplementation
Improves Organ Perfusion and Arginine Availability under Conditions with Enhanced
Arginase Activity. Nutrients. 2015 Jun 29;7(7):5217-38. doi: 10.3390/nu7075217.
PubMed PMID: 26132994; PubMed Central PMCID: PMC4516994.
2: Schwedhelm E, Maas R, Freese R, Jung D, Lukacs Z, Jambrecina A, Spickler W,
Schulze F, Böger RH. Pharmacokinetic and pharmacodynamic properties of oral
L-citrulline and L-arginine: impact on nitric oxide metabolism. Br J Clin
Pharmacol. 2008 Jan;65(1):51-9. Epub 2007 Jul 27. PubMed PMID: 17662090; PubMed
Central PMCID: PMC2291275.
3: Ware LB, Magarik JA, Wickersham N, Cunningham G, Rice TW, Christman BW,
Wheeler AP, Bernard GR, Summar ML. Low plasma citrulline levels are associated
with acute respiratory distress syndrome in patients with severe sepsis. Crit
Care. 2013 Jan 17;17(1):R10. doi: 10.1186/cc11934. PubMed PMID: 23327349; PubMed
Central PMCID: PMC4056746.
4: Cynober L. Citrulline: just a biomarker or a conditionally essential amino
acid and a pharmaconutrient in critically ill patients? Crit Care. 2013 Mar
11;17(2):122. doi: 10.1186/cc12534. PubMed PMID: 23509945; PubMed Central PMCID: PMC3672494.
5: Piton G, Manzon C, Monnet E, Cypriani B, Barbot O, Navellou JC, Carbonnel F,
Capellier G. Plasma citrulline kinetics and prognostic value in critically ill
patients. Intensive Care Med. 2010 Apr;36(4):702-6. doi:
10.1007/s00134-010-1751-6. PubMed PMID: 20084502.
6: Luiking YC, Poeze M, Ramsay G, Deutz NE. Reduced citrulline production in
sepsis is related to diminished de novo arginine and nitric oxide production. Am
J Clin Nutr. 2009 Jan;89(1):142-52. doi: 10.3945/ajcn.2007.25765. Epub 2008 Dec
3. PubMed PMID: 19056593.
7: Kao CC, Bandi V, Guntupalli KK, Wu M, Castillo L, Jahoor F. Arginine,
citrulline and nitric oxide metabolism in sepsis. Clin Sci (Lond). 2009 Jun
2;117(1):23-30. doi: 10.1042/CS20080444. PubMed PMID: 19105791.
8: Yoshitomi H, Momoo M, Ma X, Huang Y, Suguro S, Yamagishi Y, Gao M.
L-Citrulline increases hepatic sensitivity to insulin by reducing the
phosphorylation of serine 1101 in insulin receptor substrate-1. BMC Complement
Altern Med. 2015 Jun 18;15:188. doi: 10.1186/s12906-015-0706-4. PubMed PMID:
26084330; PubMed Central PMCID: PMC4472399.
9: Breuillard C, Cynober L, Moinard C. Citrulline and nitrogen homeostasis: an
overview. Amino Acids. 2015 Apr;47(4):685-91. doi: 10.1007/s00726-015-1932-2.
Epub 2015 Feb 13. Review. PubMed PMID: 25676932.
10: Vermeulen MAR, van de Pol MCG, Ligthart-Mellis GC, Dejong CHC, van den Tol P, Boelnes PG, van Leeuwen PAM. Specific amino acids in the critically ill patient-Exogenous glutamine/arginine: A Common Denominator
Are Arginine, Glutamine, and Omega 3 fatty acids Helpful?
1: van Zanten AR, Hofman Z, Heyland DK. Consequences of the REDOXS and METAPLUS Trials: The End of an Era of Glutamine and Antioxidant Supplementation for
Critically Ill Patients? JPEN J Parenter Enteral Nutr. 2015 Nov;39(8):890-2.
2: Heyland DK, Dhaliwal R. Role of glutamine supplementation in critical illness
given the results of the REDOXS study. JPEN J Parenter Enteral Nutr. 2013
Jul;37(4):442-3.
3: Vermeulen MA, Brinkmann SJ, Buijs N, Beishuizen A, Bet PM, Houdijk AP, van
Goudoever JB, van Leeuwen PA. Enteral Glutamine Administration in Critically Ill
Nonseptic Patients Does Not Trigger Arginine Synthesis. J Nutr Metab.
2016;2016:1373060.
4: 1: Chen W, Jiang H, Zhou ZY, Tao YX, Cai B, Liu J, Yang H, Lu CD, Zeng J. Is
omega-3 fatty acids enriched nutrition support safe for critical ill patients? A
systematic review and meta-analysis. Nutrients. 2014 May 30;6(6):2148-64.
5: Zhu D, Zhang Y, Li S, Gan L, Feng H, Nie W. Enteral omega-3 fatty acid
supplementation in adult patients with acute respiratory distress syndrome: a
systematic review of randomized controlled trials with meta-analysis and trial
sequential analysis. Intensive Care Med. 2014 Apr;40(4):504-12.
Review of Immunonutrition vs Standard Nutrition and Protein Supplementation in Sarcopenic Patients.
1: Volpi E, Mittendorfer B, Rasmussen BB, Wolfe RR. The response of muscle
protein anabolism to combined hyperaminoacidemia and glucose-induced
hyperinsulinemia is impaired in the elderly. J Clin Endocrinol Metab. 2000
Dec;85(12):4481-90.
2: Volpi E, Kobayashi H, Sheffield-Moore M, Mittendorfer B, Wolfe RR. Essential
amino acids are primarily responsible for the amino acid stimulation of muscle
protein anabolism in healthy elderly adults. Am J Clin Nutr. 2003
Aug;78(2):250-8. PubMed PMID: 12885705; PubMed Central PMCID: PMC3192452.
3: Bauer JM, Verlaan S, Bautmans I, Brandt K, Donini LM, Maggio M, McMurdo ME,
Mets T, Seal C, Wijers SL, Ceda GP, De Vito G, Donders G, Drey M, Greig C,
Holmbäck U, Narici M, McPhee J, Poggiogalle E, Power D, Scafoglieri A, Schultz R,
Sieber CC, Cederholm T. Effects of a vitamin D and leucine-enriched whey protein
nutritional supplement on measures of sarcopenia in older adults, the PROVIDE
study: a randomized, double-blind, placebo-controlled trial. J Am Med Dir Assoc.
2015 Sep 1;16(9):740-7.
4: Rondanelli M, Klersy C, Terracol G, Talluri J, Maugeri R, Guido D, Faliva MA,
Solerte BS, Fioravanti M, Lukaski H, Perna S. Whey protein, amino acids, and
vitamin D supplementation with physical activity increases fat-free mass and
strength, functionality, and quality of life and decreases inflammation in
sarcopenic elderly. Am J Clin Nutr. 2016 Mar;103(3):830-40.
5: Cramer JT, Cruz-Jentoft AJ, Landi F, Hickson M, Zamboni M, Pereira SL, Hustead
DS, Mustad VA. Impacts of High-Protein Oral Nutritional Supplements Among
Malnourished Men and Women with Sarcopenia: A Multicenter, Randomized,
Double-Blinded, Controlled Trial. J Am Med Dir Assoc. 2016 Nov
1;17(11):1044-1055.